Radiofrequency therapy is indicated for the treatment of neuropathic pain, neuralgia, but also persistent musculoskeletal pain such as sciatica, low back pain and neck pain, which is continuous, has an anatomically clear distribution and is resistant to conservative treatment (medicines, patches, etc.).
Neuropathic pain can be treated with the use of radiofrequency. Examples of such diseases are postherpetic neuralgia and trigeminal neuralgia.
An example of non-neuropathic pain that can be treated with radiofrequency is back pain due to degeneration of the vertebral joints, as well as selected cases of neck pain.
The use of radiofrequency is not indicated when the pain is of central etiology, i.e. the nervous system damage is located in the brain or the spinal cord.
The radiofrequencies are applied via an electrode to the active tip of a special needle, using a continuous electric field, which causes the controlled production of heat through the friction of ions. When this heat (60-90 ° C, depending on the indications) acts on a target nerve, it provokes its selective destruction and modification, with the aim of stopping the transmission of painful signals to the spinal cord and brain, thus pain relief.
The electric radio frequency field is generated by a special radio frequency generator and is applied to the target through a special needle with an active non-insulated tip. An electrode connected to the generator enters into this special needle. The generator has an indication screen and provides detailed information regarding the various parameters of the operation.
DESCRIPTION OF THE SURGERY (MAINLY CONCERNING THE SPINE)
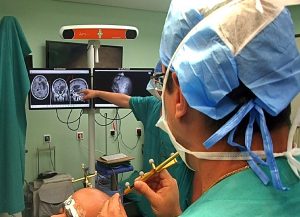
The operation is performed under local anesthesia and twilight anesthesia, with X-ray guidance (C-arm). The patient does not need to spend the night in the hospital and can go home just a few hours after the end of the operation (day care).
After all the antiseptic measures have been taken, a special needle is directed with absolute precision towards the target. We use radiographic guides, taking multiple profile, face and oblique shots, so that the needle and the electrode can navigate between the sensitive structures and away from blood vessels, the spinal cord, the dura mater and the internal organs (eg the lungs, in medial nerve access).
When the final correct position is confirmed radiographically through various shots, a contrast agent is administered to erase the contour of the nerve and its extension into the spinal canal (in case the surgery is performed inside the spine). The special electrode is then connected to the radio frequency generator.
An aesthetic test with nerve stimulation follows, using specific intensities (μA), voltages (mV) and frequencies (Hz), in order for the active tip of the needle to be placed as close to the target as possible (ie to the sensory area of the nerve). Once this is achieved and the measurements of the above parameters and tissue resistance (Ω) are satisfactory, a motor testing follows and the patient’s response to this type of stimulation is observed to ensure that the active needle tip is at a safe distance from the motor nerve that is not a target. This is a particularly delicate process if we consider that the tip of the electrode is usually 1.4 mm in diameter, while the diameter of the nerve can range from 2-5 mm. The target nerve is obviously in close proximity to the motor branch and its artery and vein, so absolute certainty is required before the treatment application, in order to avoid complications.
The electrode is then heated in a controlled selected temperature, for a few minutes (1 to 2.5 minutes, depending on the therapeutic protocol) exerting its therapeutic effect. The rise in temperature is not painful for the patient because during thermocoagulation the anesthesiologist administers twilight anesthesia and systemic central analgesia. In most cases, applying heat to a sensory nerve would be particularly painful, without continuous anesthesia. A typical operation takes 30-90 minutes, as thermocoagulation of more than one sensory branch may be required. Access may also be difficult due to anatomical abnormalities in the area (eg significant osteophytes, or anatomical variants).
RESULTS
Radiofrequency therapy is a safe and effective method of treating several chronic painful syndromes. If the pain is significantly reduced with the first application of radiofrequency then the treatment can be repeated more times. There is strong clinical evidence that radiofrequency therapy is effective in treating trigeminal neuralgia, radicular nerve pain, and spinal pain (Lord 2002). In a large study, 92.5% of patients with trigeminal neuralgia reported excellent or good relief after treatment of the trigeminal ganglion with traditional radiofrequency (Chen 2001).
The denervation of the facet joints in the lumbar and cervical spine, with the application of radiofrequency in the medial nerve branch is documented by large studies (RCT studies). A recent review for the invasive treatment of chronic spinal pain by the American Society of Interventional Pain Physicians (ASIPP) concludes that denervation of the lumbar and cervical joints of the spine is highly effective in a short period of time (3-6 months) and moderately documented for a long period of time (>>1 year).
After treatment, patients are usually relieved of the need for continuous analgesic treatment and all the possible side effects and ineffectiveness it may bring, while fully returning to their activities without any restrictions.
Especially in the case of denervation of the facet joints in the lumbar and cervical spine, the absence or reduction of pain (i.e. backache or neck pain), allows other therapeutic actions to be performed (i.e. physical therapy for muscle strengthening) which have a continuous and long-lasting effect as far as the reduction of pain episodes is concerned.