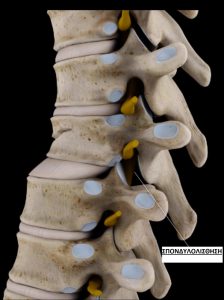
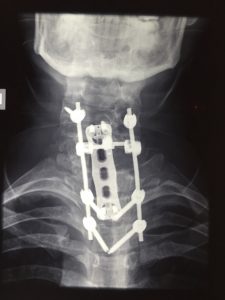
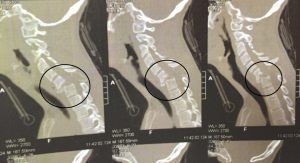
Spondylolisthesis, Spine Fractures
Percutaneous spinal fusion, immediate mobilization, without substantial post-operative pain
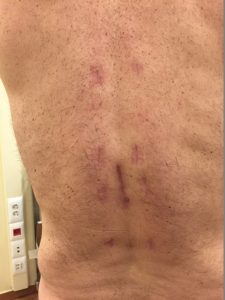
With the new technique of Minimally Invasive Spinal Surgery, fractures that need surgical stabilization become simpler and less painful. With very small incisions, similar to a laparoscopic operation, the necessary stabilization materials are placed, without substantial blood loss, and the patient is discharged in 2 days. Our experience shows that patients return to their activities pretty quickly, without any pain. Even the possibility of neurological damage caused by the injury is reduced, because these surgeries last less and the muscles, bones, and ligaments are not injured, so the recovery is faster.
Patients who have suffered a fracture or traumatic spondylolisthesis, either from a car accident, falling from a height, from osteoporosis or from a tumor of the spine , are suitable to undergo these surgeries. These surgeries are performed on the cervical, thoracic, and lumbar spine.
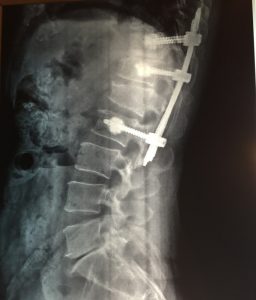
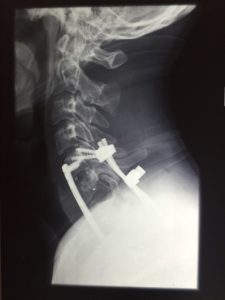
Our results are excellent, even in the most complex and “difficult” sort of speak cases, as shown in the following images from our cases:
General information about spinal cord, bone marrow, and nerve injury
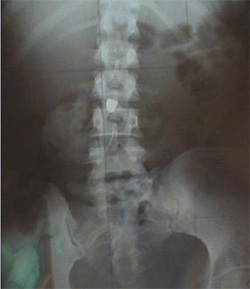 In Greece, where road safety is a well-known problem, and there is high incidence of motor vehicle accidents, there are very frequent cases of spinal injuries, especially in young and previously healthy people.
In Greece, where road safety is a well-known problem, and there is high incidence of motor vehicle accidents, there are very frequent cases of spinal injuries, especially in young and previously healthy people.
Fractures
Spinal fractures can be seen in all its parts, cervical, thoracic, lumbar, or even sacral. The higher the injury is located, the more severe the disability can be. 1/3 of the fractures are observed in the cervical spine (which is more sensitive and agile). Following a fracture, the neurological symptoms can range from minor to severe, with complete paralysis of the limbs (quadriplegia) and inability of the patient to breathe on their own. The diagnosis is made via clinical examination, history of the injury (car accident, work accident, sports accident, or criminal activity) and the imaging examinations. These include plain X-rays, CT scans, and MRI scans.
Should one opt for conservative or for surgical treatment?
There are many ways for classifying fractures. One could say that they are basically divided into stable and unstable. In the first category, surgery is not required; there is need only for pain medication and support with “splints”, i.e. collars or special corsets. However, if the fracture causes instability, surgery is required to stabilize the spine in order to protect the spinal cord and nerves.
The time when the operation is performed is also important. It has not been shown that surgery is more effective if performed a few hours after the injury. However, it needs to be carried out – with few exceptions – within 2-3 days.
Surgery may also be required if there is significant pain and disturbance in the spine architecture (significant angulation), even with no neurological deficit. Surgery may also be required if there is significant pain and disturbance in the spine architecture (significant angulation), even with no neurological deficit. Although there are numerous theoretical and experimental articles, there is still no effective way to repair the spinal cord. In the future cell implant, replacing the damaged neurons and allowing for significant neurological improvement may be possible.
Nerve injury
Injury to nerves can occur either as they exit the spine, or even further away following injuries to other bones, such as the wrist, arm, or femur. In a patient with limb weakness in one or more limbs, or any other neurological symptom, but without a proven injury to the brain, spine, or spinal cord, peripheral nerve or nerve plexus injury should be examined. A typical example is the injury of the brachial plexus after a fracture of the clavicle, which manifests itself with paralysis of the upper limb.