Neurosurgery techniques have been developed in order for operations to be performed with the least possible risk of body injury. Especially in Neurosurgery, where the object of treatment is the valuable nerve tissue, which if damaged can not be regenerated, the minimally invasive technique is really valuable for patients.
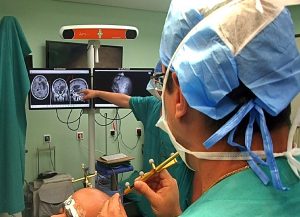
Minimally Invasive Methods utilize technologies such as Robotic Navigation, the Surgical Microscope and Endoscope , as well as a range of advanced surgical tools and equipment, such as the ultrasonic osteotomy. Surgeons who know these techniques are able to provide patients with modern surgical care in Greece, with the exact same quality characteristics as in the most advanced medical countries in the world.
Now even the most inaccessible anatomical areas can be operated on with minimal injury to sensitive nerve structures.
Minimally invasive spine surgery. Fashion or real progress?
In modern surgery, with the help of technology and the accumulation of experience, new methods have been developed, which help surgeons perform operations that in the past were particularly traumatic, with minimal risk of surgical trauma. In most surgical specialties, such as gynecology, urology, general surgery and others, the non-use of endoscopic and minimally invasive techniques for some surgeries tends to be considered bad medical practice (malpractice).
In many cases, all of these methods tend to replace open surgeries.

There is clear pressure coming from insurers, both private and public, as well as from the patients themselves for access to medical intervention which, while not lagging behind in terms of effectiveness, will be clearly more economical, and will restore the patients’ help, ensuring a better life overall.
The progress of spine surgery A typical example is spine surgeries, such as spinal fusion. Percutaneous spinal surgeries, for example, significantly reduce patients’ discomfort , pain, risk of complications, and hospitalization time. Even the largest spinal fusion does not mean that the patient is required to stay in bed. Patients with spondylolisthesis, spinal stenosis, lumbar spondylosis, and vertebral fractures after injury can move without pain within a few days and are discharged from the hospital in 2-3 days. The need for blood transfusions during spinal fusion surgeries is practically zero.
The purpose of minimally invasive techniques is to prevent injury of the muscles, blood vessels and nerves that supply them, which are caused by the conventional traditional open surgery technique. Many studies have shown that the traditional open posterior spinal fusion approach can be technically successful since X-rays show good results, but the results in terms of symptoms may be poorer than expected. The main symptoms of “Vertebral disease” are persistent back pain, the decrease in the strength of the back muscles and a feeling of fatigue or a heavy feeling in the back after performing activities. Therefore, if extensive incisions are avoided, this problem can be prevented.
Some patients who suffer from pain in the spine undergo all the necessary clinical and imaging tests (x-rays, magnetic resonance imaging, etc.) but no obvious cause of their pain is found. In order for these patients to be relieved, more specialized diagnostic and at the same time therapeutic mild invasive operations may be needed. For example nerve block, intervertebral disc herniation, joint vein denervation. All these methods are examples of minimally invasive treatments of the spine. Most of them are done using ultrasound and do not require hospitalization.
In the past, these patients would either not receive any invasive treatment and would suffer from consuming large amounts of drugs, with whatever morbidity and increase in medical costs this may cause, or they would undergo open surgery, with questionable end results and high costs.
All open vertebrae can be replaced by percutaneous, with the mere exception of surgeries to repair scoliosis. The time of full functional recovery is dramatically reduced by reducing the cost of health expenses.
Microdiscectomy becomes a matter of day care, while the incision in the skin is only 1.5 cm. The patients do not even have to spend the night in the hospital. Thus,recovery is accelated and they are able to return to their activities.
Kyphoplasty for the repair of vertebral fractures (e.g. from osteoporosis), is also done with daily hospitalization and immediate mobilization and relief of the patient.
Of course, we must be very careful in choosing the right methods. There is a risk that patients who need a normal discectomy (even in a minimally invasive way) to undergo, for example, a percutaneous disc coagulation operation, which will offer them nothing and will not avoid the discectomy. Patients are often seduced by attractive terminology (laser, robotics, bloodless, etc.). Not all cases of slipped disc are the same. Choosing the right method reduces the overall cost and inconvenience of a patient. Therefore, if minimally invasive methods are not used properly, they can harm the patient, delaying proper treatment.
Examples of Minimally Invasive Spine Surgery
|
Surgery |
Duration of Hospitalization |
Blood loss |
Postoperative chronic pain |
Type of Anesthesia |
Duration of Intervention |
| Kyphoplasty | 1 Day | 10-15 cc | 1-2 days | Intoxication | 30-60’ |
| Endoscopic Microdiscectomy | Daily | 20-30 cc | 1-2 Days | total | 60’ |
| Nerve block | Not required | 0 | 0 | Local | 20’ |
| Joint Denervation | Not required | 0 | 0 | Local / Intoxication | 20 ‘ |
| Minimally Invasive Decompression | 1 Day | 20-40 cc | 1-2 days | Total | 60-80 ‘ |
| Percutaneous Spinal Cord | 2-3 days | 40-60 cc | 2-3 days | Total | 40 ‘/ level |
| Average | <1 day | 25 cc |
1-2 days |
45 ‘ |
Comparison with Classical Invasive Methods
|
Surgery |
Duration of Hospitalization |
Blood loss |
Postoperative Pain |
Type of Anesthesia |
Duration of the operation |
| Laminectomy | 3-4 days | 100-150 cc | 7 days | total | 60-70 ‘ |
| Microdiscectomy | 1-2 days | 150 cc | 2-3 Days | total | 60′-90 ‘ |
| Trimetectomy | 2-3 days | 200 cc | 2-4 days | total | 60′-90 ‘ |
| Open Spine | 5 days | 400-600 cc | 7-10 days | Total | 60 ‘/ level |
| Average | 3 days | 250 cc |
5, 2 5 days |
75 ‘ |
Proper information of our patients contributes significantly to the selection of appropriate treatment. As surgeons, with respect to international clinical experience, we are constantly updating our techniques. Thus we harmonize with the rapidly evolving methods that improve the health of all, reducing the material and ethical costs of invasive treatment.