Fill out the form if you have an incontinence or frequent urination problem

Do you have a problem with incontinence or frequent urination? Fill in the form to find the solution together. Loading…
For the first time in Greece, a mini craniotomy operation is performed on awake patient
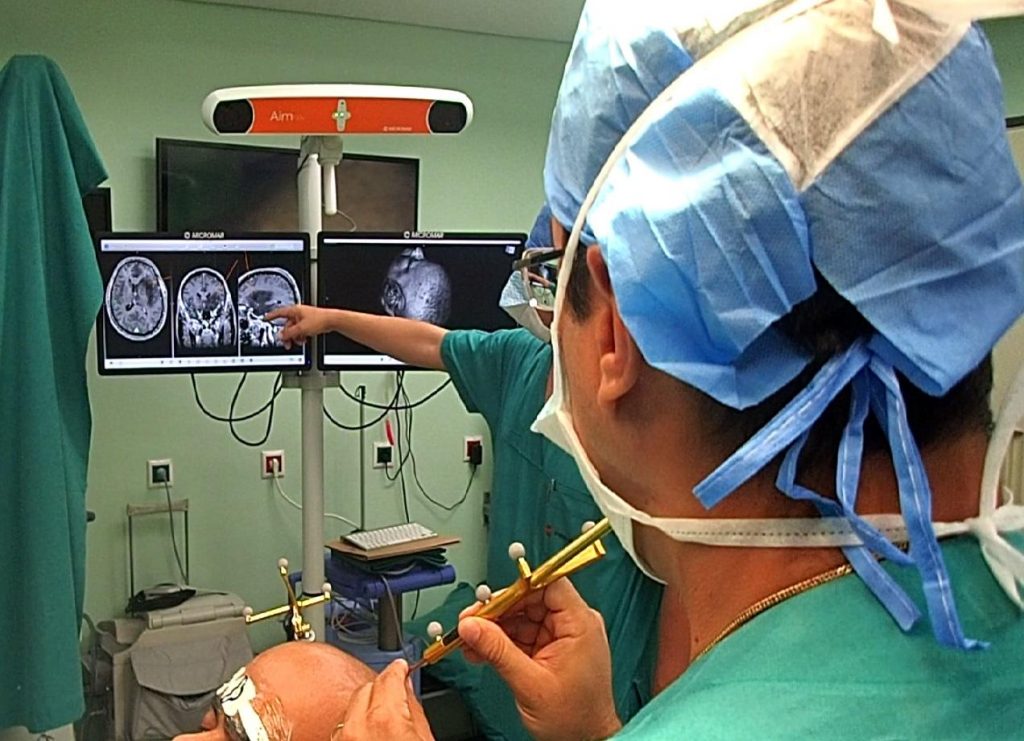
We present to you a reallyinnovative surgery that was recently performed at the Euroclinic of Athens by our Neurosurgery team, which consists of Nikolaos Maratheftis, Director Neurosurgeon, and Evangelos Rokas, Attending Neurosurgeon, on a 38 year-old male patient diagnosed with a lesion with tumor characters in the left cerebral hemisphere. This lesion spread near particularly […]
Percutaneous spine surgeries
In modern surgery, with the help of technology and the accumulation of experience, new methods have been developed, which help surgeons perform operations that in the past were particularly traumatic, with minimal risk of surgical trauma. A typical example is spine surgeries, such as spinal fusion. Percutaneous spine surgeries significantly reduce patients’ […]
Pain Treatment with Radiofrequency Electrode Application
Radiofrequency therapy is indicated for the treatment of neuropathic pain, neuralgia, but also persistent musculoskeletal pain such as sciatica, low back pain and neck pain, which is continuous, has an anatomically clear distribution and is resistant to conservative treatment (medicines, patches, etc.). Neuropathic pain can be treated with the use of radiofrequency. Examples […]
Magnetic Resonance Imaging (+ spectroscopy)
Endoscope
With the endoscope we can use a special fiber optic microcamera to see inside the tissues and direct special tools for biopsies and to investigate anatomical abnormalities, opening new drainage channels of the cerebrospinal fluid (eg 3rd ventriculostomy), opening of brain cysts , removal of pituitary tumours, removal of cerebral hematomas, and even the surgical […]

